Radiation has been a staple of cancer treatment for decades, with approximately 50 per cent of cancer patients receiving radiation therapy at some point in their journey.
While effective, traditional radiation therapies rely on intense beams of energy shot from outside the body. These beams can kill cancer cells, but their use is limited to select locations, making them less suited for difficult-to-treat metastatic cancers that have spread to multiple sites.
Now, a UBC and BC Cancer-led team of Canadian researchers has received $23.7 million in federal funding to develop a new generation of radiation therapy, known as radiopharmaceutical therapy, that delivers highly targeted doses of radiation from within.
The therapies work like a homing device — using specially designed molecules to seek out and deliver radioactive isotopes directly to cancer cells wherever they might be in the body. These radioactive warheads kill cancer with high precision, while causing minimal harm to surrounding healthy tissue and fewer side effects for patients.
 "This is the holy grail of cancer treatment. These disease-targeting molecules circulate throughout the body, binding tightly to cancer cells in order to eliminate them with a highly localized blast of energy," explained principal investigator Dr. François Bénard, senior executive director of the BC Cancer Research Institute and professor of radiology and associate dean at UBC's faculty of medicine.
"This is the holy grail of cancer treatment. These disease-targeting molecules circulate throughout the body, binding tightly to cancer cells in order to eliminate them with a highly localized blast of energy," explained principal investigator Dr. François Bénard, senior executive director of the BC Cancer Research Institute and professor of radiology and associate dean at UBC's faculty of medicine.
Radioactive isotopes emit different types of particles, ranging from relatively light beta particles (electrons) to heavier alpha particles (two neutrons and two protons). The type of particle influences how the isotope can be used, whether that's to diagnose cancer, or to treat it.
"This is the holy grail of cancer treatment. These disease-targeting molecules circulate throughout the body to eliminate cancer cells with a highly localized blast of energy," says Dr. François Bénard.
"This technique is highly adaptable to many different types of cancer and cancers that have spread to multiple locations," Dr. Bénard added. "In international studies, particularly using potent alpha emitters, we've seen incredible responses in patients with end-stage metastatic disease who had exhausted all other treatment options."
The multidisciplinary research team involves researchers from UBC, BC Cancer, TRIUMF, Simon Fraser University, Université Laval, Université de Sherbrooke, Western University, University of Toronto, University of Alberta and the Lawson Health Research Institute.
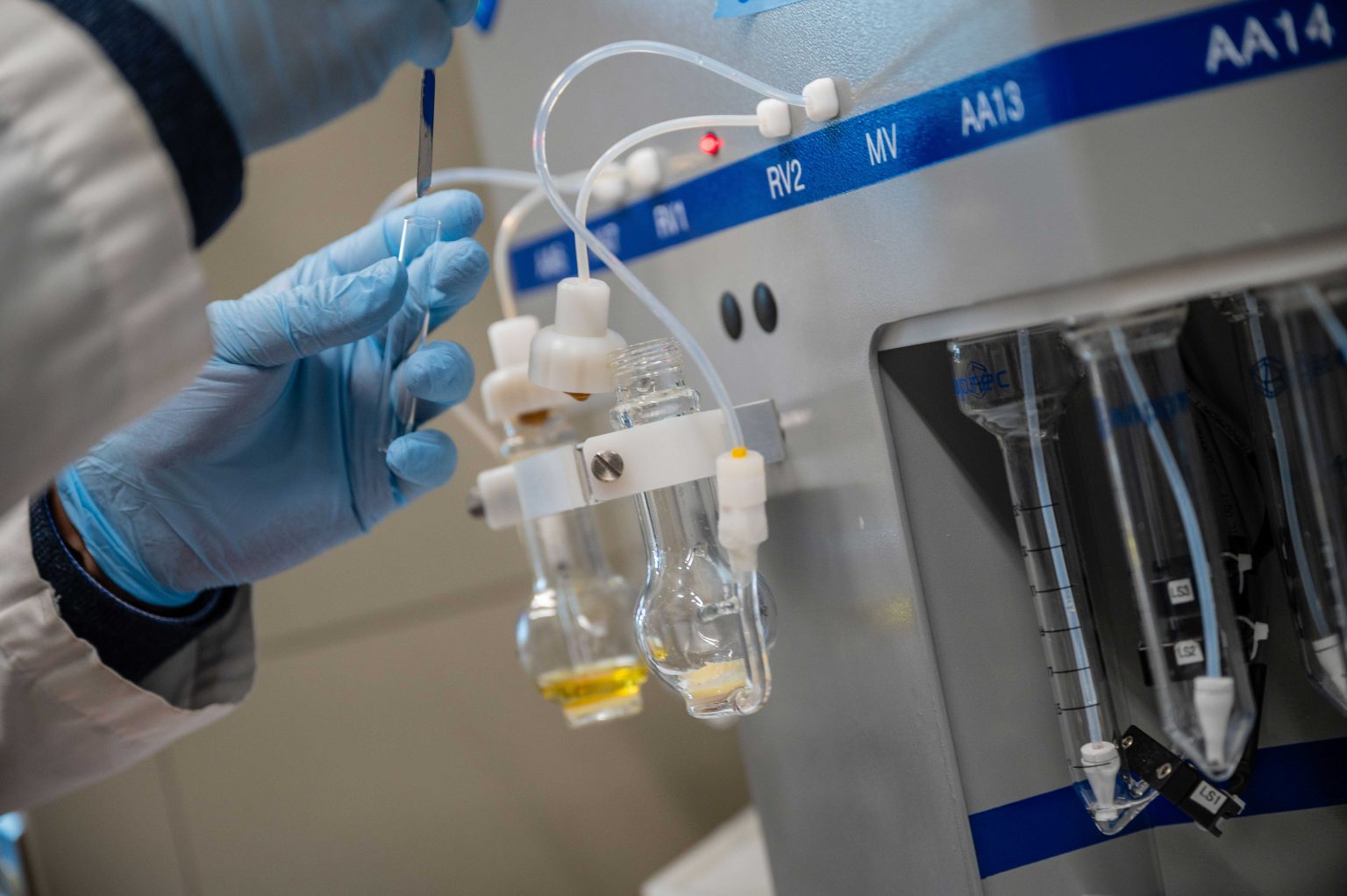
One of the key challenges they hope to overcome: a global shortage of radioisotopes. The world-wide supply of one promising element, actinium-225, is equivalent to only a few grains of sand — enough to treat no more than 2,000 patients a year.
Partnering with TRIUMF – Canada's particle accelerator centre, the team will use cyclotrons to produce clinical-grade isotopes domestically and in adequate quantities to supply Canada and the world. The team's operations will leverage TRIUMF's existing 520 MeV cyclotron, as well as new infrastructure being established within the TRIUMF-based Institute for Advanced Medical Isotopes.
"Alpha-emitting isotopes like actinium-225 have tremendous potential to change how we treat cancer, and to significantly improve health outcomes for patients," said Dr. Paul Schaffer, director, TRIUMF life sciences division. "At TRIUMF, we have unique advantages in both our world-leading isotope production facilities and our established network of collaborators within the radiopharmaceutical research and innovation ecosystem. TRIUMF is delighted to leverage its laboratory space and capabilities to ramp up and provide large quantities of rare isotopes like actinium-225, and to collaborate in the critical research taking place."
Production will initially focus on actinium-225 to meet the imminent demand for this popular radioisotope. The team will go on to establish supply chains for a library of clinically promising isotopes that can be used for therapeutic and diagnostic purposes.
The radioisotopes are attached to targeting molecules that recognize and bind to proteins on the surface of cancer cells. Another key component, known as bifunctional chelating ligands, connects the radioactive isotope to the targeting molecule and ensures its safe transport through the body.
The project is designing biomolecules to target a range of cancer types, including prostate, pancreatic, breast and blood cancers.
"Radiopharmaceutical design is intrinsically modular, which gives us the flexibility to customize each drug to a specific disease target. By considering the chemical properties of the isotope, we can design bifunctional chelating ligands that are optimised for each radioisotope and subsequently attach them to the disease targeting-molecule of our choice," said co-principal investigator Dr. Caterina Ramogida, assistant professor of chemistry at Simon Fraser University, joint with TRIUMF. "Using this adaptable approach, we have the potential to develop an arsenal of different drugs tailored for various types of cancer."
By integrating Canadian expertise in oncology, radiology, nuclear physics, nuclear engineering, chemistry, biology, clinical medicine and health economics, the project will establish a complete pipeline for the research, development and clinical translation of new radiopharmaceutical therapies.
The team hopes to bring multiple drug candidates into future clinical trials in the coming years and will accelerate their widespread adoption in Canada by navigating the regulatory compliance and economic aspects of implementing new drugs in the clinic.
"We will establish Canada as a world leader in the field of nuclear medicine and ensure Canadians and patients around the world are the ones who benefit," said Dr. Bénard. "By developing these medicines in Canada and bringing them into local clinical trials, we will ensure Canadians have access to innovative cancer treatments sooner."
Cancer remains the leading cause of death in Canada with nearly one in two Canadians expected to be diagnosed with cancer during their lifetime. One in four Canadians will die from the disease.
"Nuclear medicine has the potential to transform cancer treatment," said Dr. Bénard. "Radiopharmaceuticals can significantly improve the quality of life and life expectancy of patients with cancer, particularly metastatic cancers, many of which are currently untreatable."
*this story was repurposed, with permission, from the UBC Faculty of Medicine. Read the original version of the story here.

